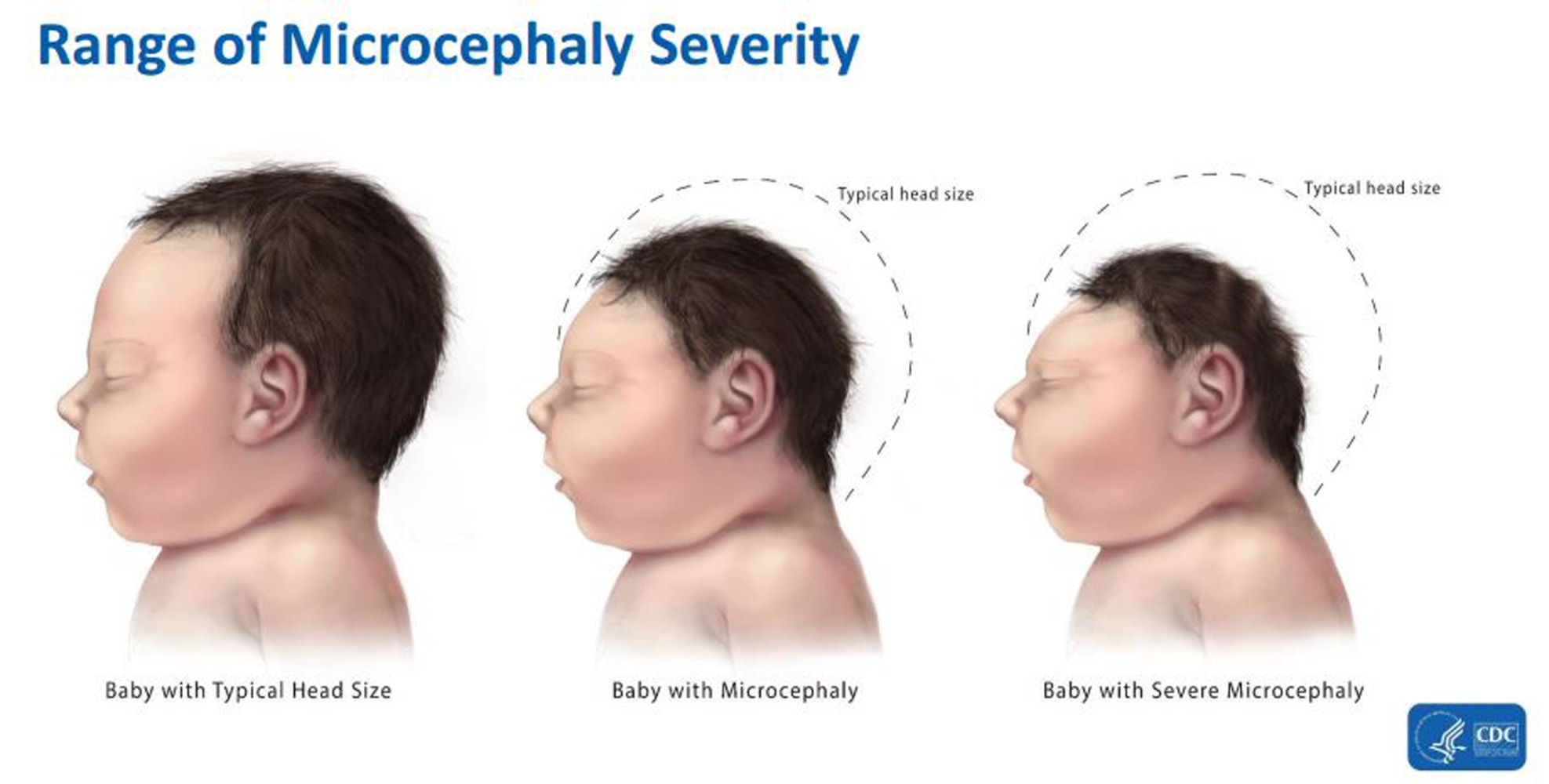
What is HPV?
Human papillomavirus (HPV) is the most common sexually transmitted infection that is easily spread through skin-to-skin contact. There are over 100 different strands of the virus that are identified as low-risk (minor abnormalities at the cervix and genital warts) or high-risk (precursor lesions and cancer). High-risk types of HPV are the cause of cervical cancer and can also be associated with cancer of the vulva, anus, oropharynx, and penis. Although every case of cervical cancer is caused by HPV, not every type of HPV causes cervical cancer.
Who can get HPV?
It is estimated that 79 million Americans are infected by HPV. Almost all males and females will be infected by at least one strand of HPV at some point in their lives.

How do you know if you have HPV?
Developing genital warts is one way to diagnose HPV. HPV can also be detected during a female’s annual PAP test. If a female has an abnormal PAP smear, the doctor may then perform an DNA test by swabbing the cervix to identify the type of HPV or a colposcopy which involves examining the cervix, vagina, and vulva with a magnifying device.
Is there a cure?
There is currently no cure for HPV. However, most cases of HPV resolve on their own within 2-3 years.
How can you prevent getting HPV?
The use of condoms provides only 60% protection against HPV because it can still be sexually transmitted through unprotected genital skin areas. The only primary prevention method among sexually active individuals is to obtain an HPV vaccine.
There are three HPV vaccines, Gardasil, Gardasil 9, and Cervarix. They all protect against HPV types 16 and 18, which cause 7 out of 10 cases of cervical cancer. Gardasil and Gardasil 9 also protect against types 6 and 11, which cause 9 out of 10 cases of genital warts. Gardasil 9 protects against an additional 5 strains of HPV which can cause cervical, vulvar, vaginal, and anal cancer.
Who should get the HPV vaccine?
Ideally, you should get the vaccine before becoming sexually active. However, people who have had sex can also benefit from getting the vaccine. It is recommended that all girls and women ages 9 to 26 get an HPV vaccine. Boys and men ages 9 to 26 can get the vaccine to prevent genital warts, some cancers of the anus and mouth/throat, and to prevent the spread of HPV to women which could potentially cause cancer.

Is the vaccine safe?
There is no live virus in any of the HPV vaccines, so they can not give you an infection. The vaccines make your body’s immune system produce antibodies to certain HPV types which protect you from getting infected with HPV. The most common side effects of the vaccines are bruising, itching, redness, swelling, or tenderness around the area where the shot is given. Women may also experience dizziness, fainting, mild fever, nausea, and vomiting. If you happen to experience any of these symptoms they typically do not last long and usually pass on their own.
Does the vaccine promote sexual activity?
Studies have shown that sexual activity among people who have received the vaccine did not differ from those who did not receive the vaccine. Studies have also shown that people who had gotten the vaccine were actually more aware of the need to practice safer sex than those who did not get the vaccine.
The HPV vaccine does not protect against all types of HPV that can cause cancer. Therefore, it is important to still get routine Pap tests.
For more information you can visit these websites:
Centers for Disease Control and Prevention
References Souho, T., Benlemlih, M., & Bennani, B. (2015). Human Papillomavirus Infection and Fertility Alteration: A Systematic Review. Plos ONE, 10(5), 1-9. doi:10.1371/journal.pone.0126936 Marek, E., Dergez, T., Bozsa, S., Gocze, K., Rebek-Nagy, G., Kricskovics, A., & ... Gocze, P. (2011). Incomplete knowledge - unclarified roles in sex education: results of a national survey about human papillomavirus infections. European Journal Of Cancer Care, 20(6), 759-768. doi:10.1111/j.1365-2354.2011.01258.x Krawczyk, A., Lau, E., Perez, S., Delisle, V., Amsel, R., & Rosberger, Z. (2012). How to Inform: Comparing Written and Video Education Interventions to Increase Human Papillomavirus Knowledge and Vaccination Intentions in Young Adults. Journal Of American College Health, 60(4), 316-322. doi:10.1080/07448481.2011.615355 Ratanasiripong, N. T. (2014). Human Papillomavirus Vaccine Increases High-Risk Sexual Behaviors: A Myth or Valid Concern. Journal Of School Nursing (Sage Publications Inc.), 30(6), 456-463. doi:10.1177/1059840513520042 Barnack-Tavlaris, J. L., Garcini, L., Sanchez, O., Hernandez, I., & Navarro, A. M. (2013). Focus Group Discussions in Community-Based Participatory Research to Inform the Development of a Human Papillomavirus (HPV) Educational Intervention for Latinas in San Diego. Journal Of Cancer Education, 28(4), 784-789. doi:10.1007/s13187-013-0516-7

/about/midsection-of-pregnant-woman-standing-at-forest-601250315-57704aee5f9b585875c1d15a.jpg)